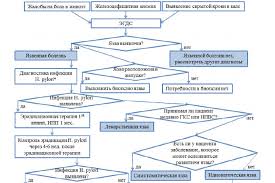
COMBINED COMPLICATIONS OF DUD: A NEW CLASSIFICATION AND PATHOGENETIC STRATEGY
At the beginning of the 21st century, the structure of duodenal ulcer disease (DUD) underwent a significant pathomorphological transformation. Against the backdrop of the widespread implementation of modern eradication therapy, a paradoxical shift occurred: the number of elective surgeries decreased, while the proportion of hospital admissions with combined complications (CC) critically increased. The concurrence of such aggressive forms as bleeding, perforation, stenosis, and penetration gives rise to a “mutual aggravation syndrome,” turning diagnosis and the choice of surgical strategy into an extremely complex challenge. The absence of a unified classification and a clear understanding of the pathogenetic sequence has, until now, resulted in unacceptably high mortality rates (ranging from 15% to 50%, depending on the combination of factors).
The high incidence of diagnostic and tactical errors in cases of combined complications of DUD underscores the urgent need to develop a pathogenetically grounded classification that would serve as a platform for creating standardized diagnostic and therapeutic protocols and optimizing the selection of the appropriate extent of surgical intervention.
We have proposed a variant classification and a pathogenetic model for the development of combined complications of duodenal ulcer disease (DUD) based on the analysis of treatment outcomes in 658 patients.
The treatment results of 658 patients with combined complications (CC) of DUD were analyzed. The most frequent combination was stenosis associated with penetration — 368 cases (56.1%). A long-standing disease history (up to 27 years) was noted in 81.7% of patients. A comprehensive diagnostic approach was applied, including endoscopy (Forrest classification), radiological examination, and intraoperative assessment of the gastroduodenal zone, with mandatory consideration of the Mannheim Peritonitis Index (MPI) and surgical risk prediction.
The main pathogenetic concept was based on our hypothesis regarding the role of penetration as the trigger and key initiating mechanism in the majority (cascade) of complications.
A working classification has been proposed, dividing patients into four groups according to the predominant complication:
Group I (Chronic Complications):
Stenosis + penetration. Cicatricial (scar-related) changes predominate.
Group II (Chronic + Acute):
Stenosis and penetration complicated by bleeding or perforation. This represents the most challenging category in terms of determining the appropriate surgical strategy.
Group III (Binary Acute Complications):
Perforation + bleeding. These cases require emergency simultaneous hemostasis and elimination of peritonitis.
Group IV (Multiple and Rare Complications):
Combination of more than three complications or involvement of adjacent structures (biliodigestive fistulas, common bile duct stricture, pancreatitis).
We strongly advocate a strictly differentiated approach:
- In chronic complications (Group I): planned (elective) surgery after correction of homeostasis.
- In acute complications (Groups II–III): priority management of life-threatening conditions (hemostasis, control of peritonitis) with simultaneous restoration of duodenal patency.
- An important determinant of success is consideration of concomitant duodenal outflow disorders (chronic duodenal obstruction).
Conclusion.
The development of complications of duodenal ulcer disease represents a unified pathogenetic destructive process, realized through penetration. The proposed classification makes it possible to systematize tactical approaches and standardize the selection of the surgical volume, which is a necessary prerequisite for reducing postoperative mortality.
Saidaliev Sh.Sh., MD, PhD
Associate Professor, Department of Surgical Diseases № 1